Our services
Request an appointment
Reserve your spot with our medical team in just minutes.
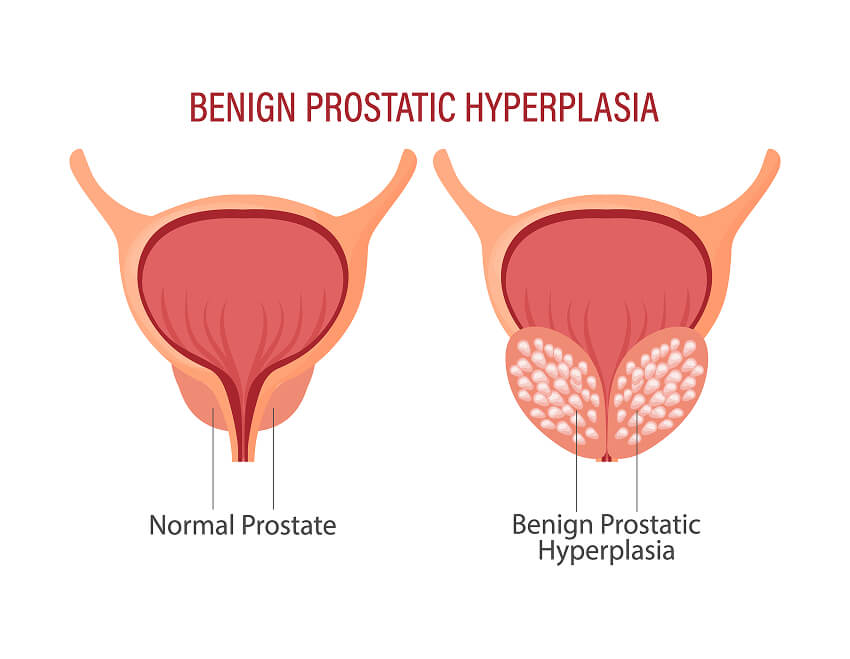
How Common Is Prostate Enlargement (BPH) and Why Should Men Pay Attention?
Benign Prostatic Hyperplasia (BPH), commonly known as prostate enlargement, is one of the most frequent urological conditions affecting aging men. By the age of 50, nearly half of men show signs of prostate enlargement, and this number increases significantly with age. While BPH is not cancerous, it can seriously affect quality of life if left untreated.
Many men initially ignore symptoms, assuming urinary changes are a normal part of aging. However, early evaluation and timely treatment can prevent complications such as urinary retention, infections, and kidney damage.
Understanding how prostate disease is diagnosed and treated helps men seek care before symptoms worsen.
What Are the Early Signs That Suggest Prostate Disease or BPH?
Prostate enlargement usually presents with lower urinary tract symptoms (LUTS), which may develop gradually or appear suddenly.
Common symptoms include:
In some cases, BPH may be detected incidentally during routine health check-ups, even before symptoms become bothersome.
How Is Prostate Enlargement (BPH) Diagnosed by a Urologist?
When BPH is suspected, the urologist takes a step-by-step approach to understand what’s really causing the symptoms. The goal is to confirm prostate enlargement while also making sure there isn’t an infection or something more serious causing similar problems.
Clinical Examination and Initial Assessment
Digital Rectal Examination (DRE) of the Prostate
During this clinic-based examination, the urologist gently inserts a gloved finger into the rectum to assess:
This simple examination provides valuable information and helps guide further tests.
DRE remains a cornerstone of prostate assessment.
What Laboratory Tests Are Needed to Evaluate Prostate Problems?
To understand prostate problems better, doctors often start with a few basic lab tests. These tests help rule out infection, check prostate health, and guide the next steps in treatment, without anything complicated or painful. Blood and urine tests help assess infection, kidney function, and cancer risk.
Commonly advised tests include:
Understanding PSA Testing
PSA is a protein produced by prostate cells. Elevated levels may be seen in:
PSA testing is also used to monitor patients after prostate cancer treatment.
PSA results are always interpreted in combination with clinical findings.
Which Imaging Tests Help Confirm BPH and Its Severity?
Imaging tests help doctors see the size of the prostate, check the health of the bladder, and find out if urine is getting left behind instead of emptying properly.
Ultrasound of Abdomen and Pelvis
An Ultrasound of the Abdomen and Pelvis is really important as it:
TRUS (Transrectal Ultrasound)
TRUS provides a closer and more detailed view of:
These tests help plan treatment and rule out serious pathology.
How Is Urine Flow Assessed in BPH Patients?
Uroflowmetry is an easy, painless test that checks how strong and smooth your urine flow is when you pass urine.
What Happens During Uroflowmetry?
This test helps quantify symptom severity and monitor treatment response.
Objective measurement improves treatment accuracy.
Why Is Cystoscopy Sometimes Needed in Prostate Evaluation?
Cystoscopy allows direct visualisation of the urinary passage.
Role of Cystoscopy in BPH
It is performed under local or general anaesthesia and provides valuable diagnostic clarity.
Cystoscopy is especially helpful before surgical planning.
What Are the Different Types of Prostatitis?
Not all prostate problems are due to enlargement. Prostatitis is inflammation of the prostate and has distinct types.
Acute Bacterial Prostatitis
Treatment involves antibiotics and supportive care.
Chronic Bacterial Prostatitis
Requires prolonged antibiotic therapy.
Chronic Prostatitis / Chronic Pelvic Pain Syndrome
Management focuses on symptom control.
Asymptomatic Prostatitis
Accurate diagnosis ensures correct treatment and avoids unnecessary procedures.
How Is Benign Prostatic Hyperplasia (BPH) Treated?
Treatment depends on symptom severity and impact on daily life.
When Is Medical Treatment for BPH Appropriate?
Mild to moderate symptoms may respond well to medications.
Common medications include:
Medical therapy can provide relief but is not suitable for all patients.
Prolonged medication should not delay surgery when clearly needed.
When Is Surgery Recommended for BPH?
Surgery is advised when:
What Is TURP and Why Is It the Gold Standard for BPH?
Transurethral Resection of the Prostate (TURP) is the most established surgical treatment for BPH.
Here’s How TURP Works:
More than 90% of prostate surgeries are performed using this method.
TURP offers long-term symptom relief with proven results.
What Role Does Laser Surgery Play in Prostate Treatment?
Laser prostate surgery is increasingly used, especially for larger glands.
Holmium Laser Enucleation (HoLEP)
Laser surgery requires anaesthesia and short hospital stay.
Laser techniques are safe, precise, and effective in expert hands.
When Is Open Prostate Surgery Needed?
Open surgery is rarely required today but may be necessary when:
The surgeon removes enlarged tissue through an incision under anaesthesia.
Open surgery is reserved for complex and select cases only.
Why Timely Prostate Evaluation and Treatment Matters?
Prostate diseases are common, manageable, and highly treatable when diagnosed early. Ignoring urinary symptoms can lead to serious complications. With modern diagnostics, medications, and minimally invasive surgeries, men can regain comfortable urination and quality of life.
